You've been trying. You track your cycle, maybe you've even bought the ovulation kits. But month after month, that single line or the arrival of your period feels like a punch in the gut. If this sounds familiar, you're not alone. Fertility issues in women are far more common than most people realize, affecting roughly 1 in 8 couples. The journey can feel isolating, confusing, and overwhelmingly medical. But here's the thing I've learned after years of working with women navigating this path: understanding what's happening in your body is the first, most powerful step toward finding a solution. This isn't just about biology; it's about reclaiming a sense of agency in a process that often makes you feel powerless.
What's Inside This Guide?
- What Are the Most Common Female Fertility Issues?
- The Hidden Signs: Are You Missing These Clues?
- The Diagnosis Path: What to Expect at the Doctor's Office
- How to Improve Female Fertility Naturally (Beyond the Broccoli)
- When Nature Needs a Nudge: Exploring Medical Options
- Your Fertility Questions, Answered Honestly
What Are the Most Common Female Fertility Issues?
Let's cut through the jargon. When doctors talk about female infertility causes, they're usually grouping them into a few key buckets. The mistake many make is thinking it's one single thing. More often, it's a combination of factors quietly stacking the odds against you.
| Category of Issue | Primary Causes & Examples | How It Affects Conception |
|---|---|---|
| Ovulation Disorders | PCOS (Polycystic Ovary Syndrome), hypothalamic dysfunction, premature ovarian insufficiency, high prolactin. | No egg is released, or release is irregular/unpredictable. This is one of the most frequent culprits. |
| Tubal & Uterine Factors | Blocked fallopian tubes (from past infection, endometriosis), uterine fibroids, polyps, scar tissue (Asherman's syndrome). | Blocks sperm from reaching the egg, prevents embryo implantation, or increases miscarriage risk. |
| Endometriosis | Growth of uterine-like tissue outside the uterus, often on ovaries, tubes, and pelvic lining. | Creates inflammation, scar tissue, and a hostile pelvic environment that can disrupt ovulation, fertilization, and implantation. |
| Cervical & Unexplained | Hostile cervical mucus, sperm antibodies. Unexplained infertility (all tests normal). | Sperm can't swim through the cervix. Unexplained cases are frustrating but account for 15-30% of diagnoses. |
Look at PCOS for a second. It's not just "irregular periods." It's a metabolic and hormonal rollercoaster where your ovaries get crowded with tiny follicles that don't mature properly. Insulin resistance often plays a huge role here, something many OB/GYNs still don't emphasize enough during initial conversations.
A quick note on age: Yes, it's a factor. Egg quantity and quality naturally decline, most notably after 35. But framing it as just a "biological clock" panic is unhelpful. It's about probability. A 30-year-old has about a 20% chance per cycle. By 40, it's around 5%. This doesn't mean impossible, it means the efficiency of the system changes, and underlying issues become more critical to identify quickly.
The Hidden Signs: Are You Missing These Clues?
Signs of fertility problems in women aren't always the obvious "I can't get pregnant." Your body sends signals long before you start trying. We often dismiss them as just "how my body is."
Your Menstrual Cycle is the Best Report Card
Forget just marking the first day. Become a detective.
Cycle Length: Consistently shorter than 21 days or longer than 35 days can point to ovulation issues. I see women celebrating a "regular" 40-day cycle, not realizing ovulation might be absent or very late.
Flow and Pain: Periods so heavy you change protection hourly, or pelvic pain that radiates to your back/thighs and isn't relieved by ibuprofen, can be red flags for conditions like fibroids or endometriosis. Severe pain is not normal.
Missing the Mid-Changes: Do you get that clear, stretchy egg-white cervical mucus around day 14? Its absence can indicate poor estrogen production or cervical factors.
The Symptoms You Brush Aside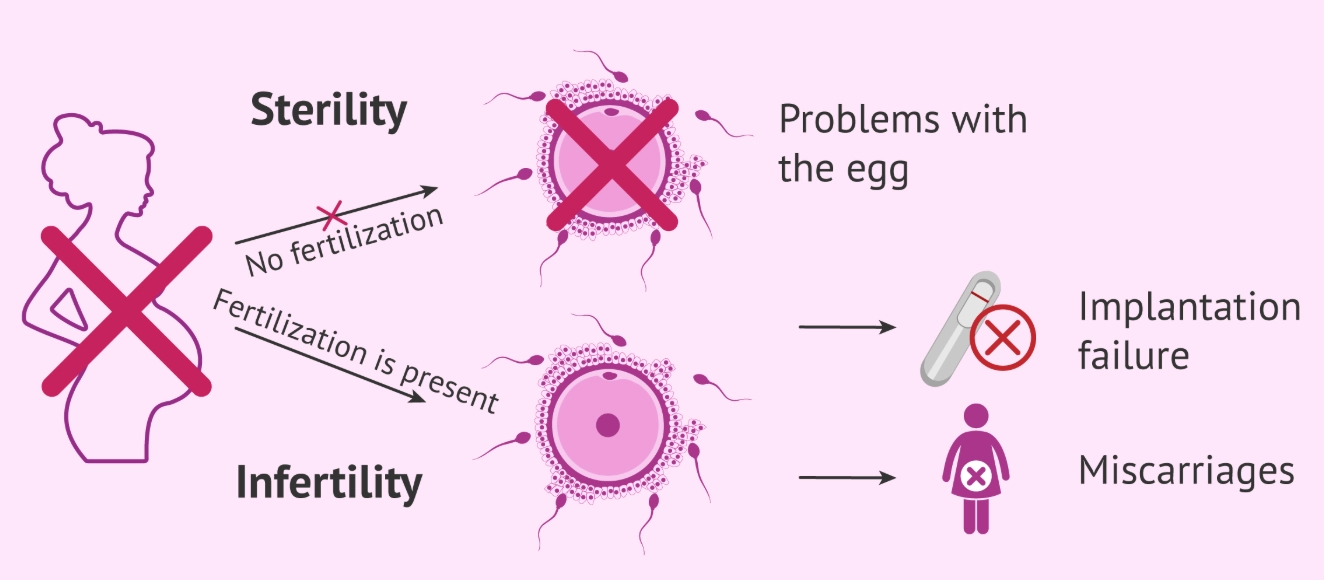
Unwanted hair growth on your face/chest, sudden acne in your 30s, or thinning scalp hair can suggest high androgens, classic in PCOS. Unexplained weight gain that's stubborn to lose, especially around the middle, ties back to that insulin resistance piece. Pain during or after sex isn't just a nuisance; it can be a sign of endometriosis or pelvic inflammatory disease.
The Diagnosis Path: What to Expect at the Doctor's Office
So you've decided to seek help. The standard workup usually follows a logical sequence. Don't be intimidated; think of it as gathering data.
First, the Conversation: A good doctor will take a deep dive into your history: cycle details, past pregnancies, surgeries, infections, lifestyle, even your mother's age at menopause.
The Basic Tests:
- Day 3 Hormone Panel: FSH, LH, Estradiol, AMH (Anti-Müllerian Hormone). AMH gives an estimate of your ovarian reserve, but it's not a fertility crystal ball. A low AMH with a high FSH suggests diminished reserve.
- Ovulation Confirmation: A mid-luteal phase progesterone blood test (7 days post-ovulation).
- Imaging: A transvaginal ultrasound looks at your ovarian follicles, uterine shape, and checks for fibroids or cysts.
- The HSG (Hysterosalpingogram): An X-ray where dye is injected into your uterus and tubes. It checks for blockages and uterine abnormalities. It can be uncomfortable, but it's over quickly.
Resources like the American Society for Reproductive Medicine (ASRM) have great patient guides on these tests. The CDC also publishes annual data on fertility clinic success rates, which is useful later if you need treatment.
How to Improve Female Fertility Naturally (Beyond the Broccoli)
Everyone Googles "improving female fertility naturally." You'll find a million posts about kale and acupuncture. Some of it helps, some is noise. Let's focus on what moves the needle based on the science and what I've seen work.
Nutrition: It's About Blood Sugar, Not Just Folate
Yes, take a prenatal with folate. But the bigger game-changer is stabilizing your insulin. High insulin disrupts ovulation and worsens PCOS.
Actionable Steps: Pair every carb with a protein and fat. Swap white bread/pasta for whole grains. Add cinnamon to your diet (it's shown to improve insulin sensitivity). Reduce added sugar and sugary drinks dramatically. This isn't about weight loss per se; it's about hormone regulation. I've seen cycle regularity return just from these dietary shifts alone.
Lifestyle Tweaks That Actually Matter
Sleep: Chronic poor sleep raises cortisol, which can suppress ovulation. Prioritize 7-8 hours. It's non-negotiable.
Exercise: The Goldilocks rule. Intense, daily marathon training can hurt fertility. Being sedentary is just as bad. Aim for moderate movement 30 minutes most days—brisk walking, swimming, yoga. It reduces inflammation and improves blood flow.
Stress Management: Don't roll your eyes. Chronic stress affects the hypothalamic-pituitary-ovarian axis. It's biology. Find what works for you—10 minutes of meditation, journaling, walking in nature. It's not about eliminating stress (impossible), but about changing your body's response to it.
Environmental Toxins: This is the under-discussed one. Swap plastic food containers for glass. Avoid BPA, phthalates (in scented products, soft plastics). Choose clean personal care products. The data linking these endocrine disruptors to fertility is growing.
When Nature Needs a Nudge: Exploring Medical Options
If lifestyle and basic interventions aren't enough after 6-12 months (or sooner if you're over 35 or have a known issue), medical treatments are the next step. This isn't failure; it's using the right tools for the job.
Medications: Clomiphene citrate or Letrozole are oral drugs that stimulate ovulation. They're often the first-line treatment for ovulation disorders like PCOS. Monitoring with ultrasound is crucial to avoid over-response.
Intrauterine Insemination (IUI): Washed sperm is placed directly into the uterus around ovulation. It bypasses cervical issues and increases sperm concentration near the egg. Success rates per cycle are modest (10-20%), but it's less invasive and expensive than IVF.
In Vitro Fertilization (IVF): Eggs are retrieved, fertilized in a lab, and resulting embryos are transferred to the uterus. It's the most effective treatment for blocked tubes, severe male factor, endometriosis, and unexplained infertility. It's also a major physical, emotional, and financial commitment. Success depends heavily on age and clinic expertise.
Surgery: Laparoscopic surgery can remove endometriosis lesions, open blocked tubes, or remove fibroids. It's diagnostic and therapeutic.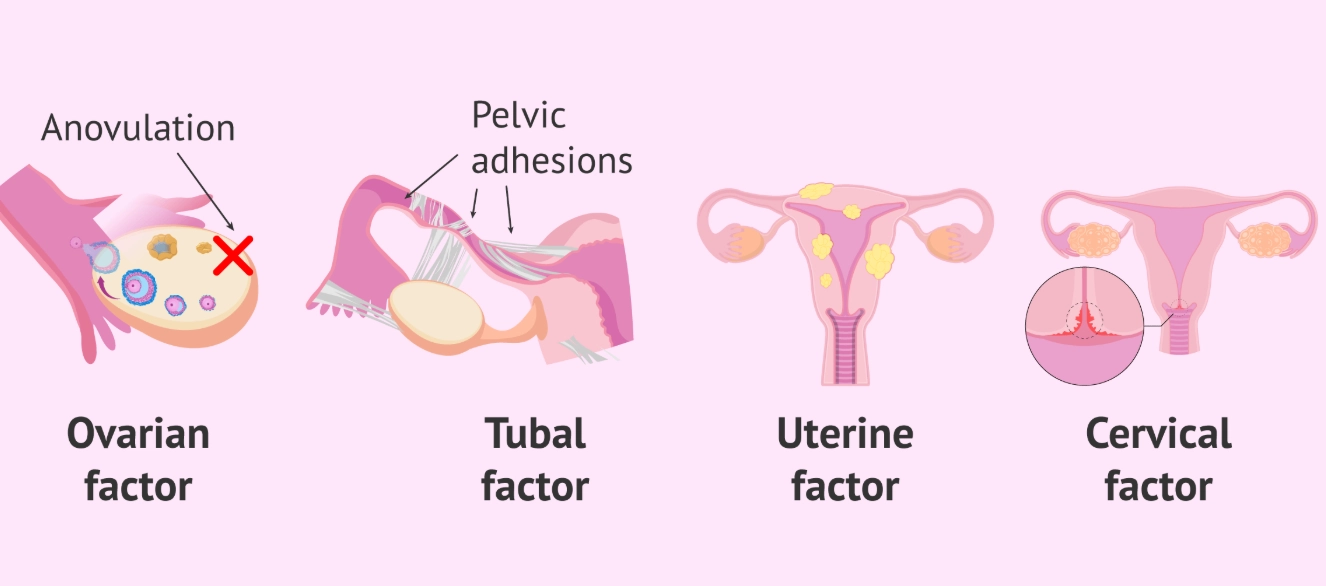
Your Fertility Questions, Answered Honestly
 Are all those over-the-counter fertility supplements and teas worth the money?
Are all those over-the-counter fertility supplements and teas worth the money?The path through fertility challenges is rarely straight. It's okay to feel overwhelmed, angry, or sad. The goal isn't to become a perfect fertility machine, but to become an informed advocate for your own health. Gather your data, ask the tough questions, and build a support team—a compassionate doctor, a partner who's in the trenches with you, maybe a therapist or a support group. Your journey is unique, but you don't have to walk it alone.





Leave a comment