Let's talk about the birth control pill. It's one of the most common forms of contraception, but it's also surrounded by a cloud of questions and myths. Is it right for you? Which one? What about the side effects everyone whispers about? I've spent over a decade talking to gynecologists, pharmacists, and hundreds of women about their experiences with oral contraceptives. The biggest mistake I see? People treat all pills as the same and get frustrated when their experience doesn't match the textbook description. This guide will cut through the noise. We'll go beyond the basics into the practical realities of choosing, using, and living with the pill.
What's Inside This Guide
How Do I Choose the Right Birth Control Pill?
Walking into a doctor's office and just accepting whatever pill they prescribe is like buying the first car you see on the lot. You need to know what's under the hood. The two main categories are combination pills (containing estrogen and progestin) and progestin-only pills (often called the "mini-pill").
Here’s the breakdown most websites don't give you clearly:
| Type of Pill | Key Hormones | Best For... | Common Brand Examples* | Considerations |
|---|---|---|---|---|
| Combination Pill (Monophasic) | Estrogen + Progestin (steady dose) | First-time users, regular cycles, acne control. | Yaz, Lo Loestrin Fe, Apri | Most common type. May help with PMS and heavy flow. |
| Combination Pill (Multiphasic) | Estrogen + Progestin (varying doses) | Women who have breakthrough bleeding on monophasic pills. | Ortho Tri-Cyclen, Estrostep Fe | Tries to mimic a natural cycle; can be trickier if you miss a pill. |
| Progestin-Only Pill (Mini-Pill) | Progestin only | Breastfeeding moms, those who can't take estrogen (due to migraines with aura, high blood pressure, smoking over 35). | Slynd, Camila, Heather | Must be taken at the exact same time every day (3-hour window max). Less impact on milk supply. |
*Brand names are for reference; generics are widely available and equally effective.
A specific non-consensus point here: Many doctors default to ultra-low-dose estrogen pills (like Lo Loestrin Fe) thinking they have fewer side effects. While sometimes true, they also have a higher chance of causing breakthrough bleeding—random spotting that can last for months. For some women, a slightly higher, standard-dose pill actually provides more cycle stability with minimal side effect difference. It's a trade-off you should discuss.
Your choice isn't just about preventing pregnancy. Are you looking to clear up hormonal acne? Regulate wildly unpredictable periods? Reduce crippling menstrual cramps? These are valid goals. Tell your doctor. A pill like Yaz or Estrostep Fe is specifically FDA-approved for acne because of its particular progestin.
What Are the Most Common Side Effects and How Can I Manage Them?
Let's be real. Side effects are the main reason people give up on the pill. But often, it's because they weren't prepared or didn't know when to ride it out versus when to switch.
The First 3 Months: The Adjustment Period
Your body is adapting to new hormone levels. Nausea, breast tenderness, mood swings, and spotting are very common. I tell my friends to give it a solid 3-month trial unless side effects are severe (like debilitating migraines). The nausea often fades if you take the pill with dinner or just before bed.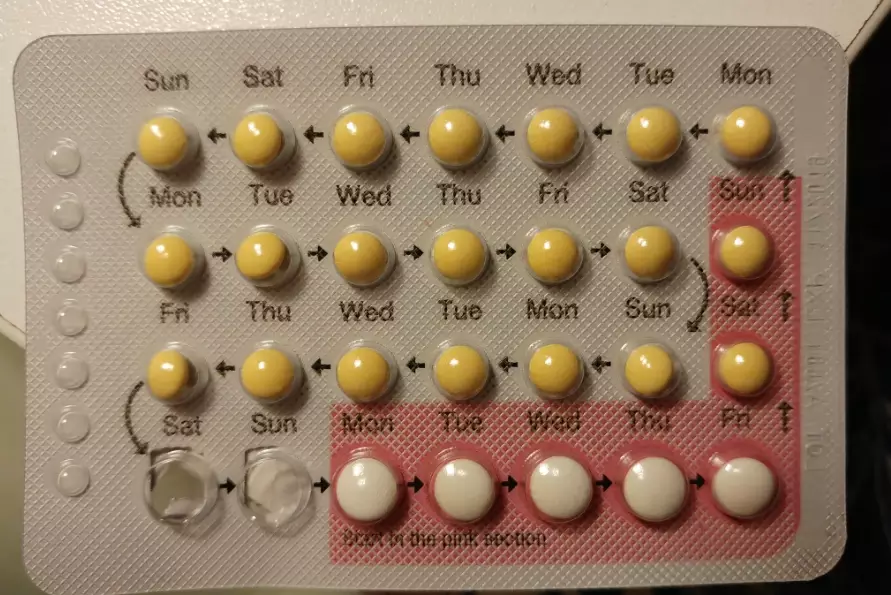
Beyond the Basics: Weight and Mood
Here's the expert nuance: The pill rarely causes significant fat gain. What it often causes is fluid retention (bloat) and can increase appetite. The scale might go up 2-5 pounds from water. Managing salt intake and staying hydrated can help more than you think.
Mood changes are trickier. Some pills can worsen underlying anxiety or depression. If you feel persistently sad, irritable, or "flat" after the adjustment period, don't dismiss it as "just you." Talk to your doctor. Switching to a different progestin (like from levonorgestrel to drospirenone) can make a world of difference. It's not one-size-fits-all.
How to Take the Pill Correctly for Maximum Effectiveness
That "99% effective" rate you hear about? That's with perfect use. Typical use, with human error, drops it to around 91%. The gap is all about the details.
For combination pills: You have a 12-hour window to take it and still be considered "on time." But consistency is key. Set a phone alarm linked to a daily habit (like brushing your teeth). If you miss that window, take it as soon as you remember. If you're more than 24 hours late, you've missed a pill. Take the missed one immediately, take today's pill at the usual time (you might take two in one day), and use backup contraception (condoms) for the next 7 days.
For the progestin-only mini-pill: This is non-negotiable. You have a 3-hour window. Miss it, and you need to take the missed pill ASAP, use backup for 2 days, and maybe take emergency contraception if you had sex in the previous 48 hours. It's much less forgiving.
A real-life scenario: You get food poisoning or severe diarrhea. That can interfere with absorption. The rule of thumb is if you have vomiting within 3-4 hours of taking the pill, or severe diarrhea for more than 24 hours, treat it as a missed pill. Use backup.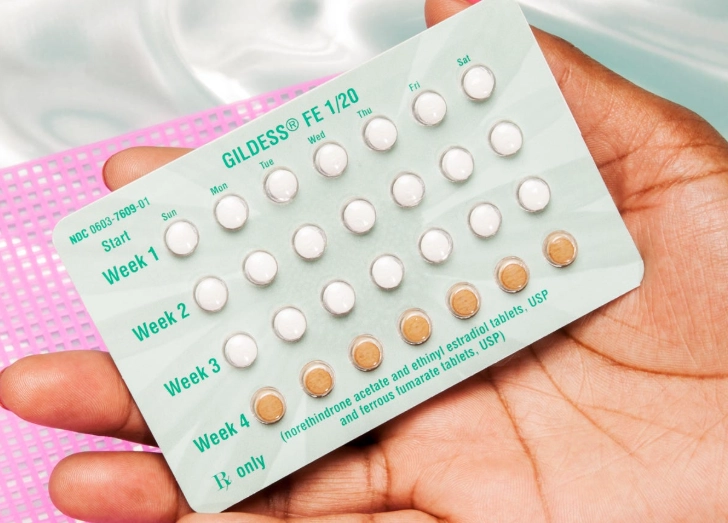
Thinking Long-Term: What You Need to Know
You've been on the pill for years. Is that okay? For most healthy, non-smoking women, yes. Long-term studies, like those cited by the CDC, show it's safe for extended use. You don't need to "take a break" to "cleanse" your body—that's a myth and can lead to unintended pregnancy.
What about interactions? The big one is certain antibiotics. The only antibiotic proven to reduce pill effectiveness is rifampin (used for tuberculosis). For common antibiotics like amoxicillin for a sinus infection, the evidence is shaky, but many pharmacists and doctors still recommend backup protection to be ultra-safe. Always ask.
Other culprits: The herbal supplement St. John's Wort, some anti-seizure medications, and some HIV treatments. When in doubt, tell every healthcare provider you're on the pill.
Your Questions, Answered
I always forget to take my pill on time. What should I do?
First, be honest with yourself. If you're missing more than one pill a month, the pill might not be the right method for you. Consider a "set it and forget it" method like an IUD or implant. If you want to stick with it, move the pill pack next to your toothbrush or phone charger. Use an alarm with a label that says "PILL" not just a generic beep. If you miss often, ask your doctor about a continuous-cycle pill (with no placebo weeks) so you have fewer periods and potentially fewer packs to manage per year.
Does the birth control pill make it harder to get pregnant later?
No. This is a persistent fear with no scientific backing. Fertility returns quickly after stopping most pills. For some, it might take a few months for cycles to regulate, but long-term studies show no difference in the ability to conceive compared to women who never used hormonal contraception. Your age when you stop is a far bigger factor than your past pill use.
I'm on the pill and had unprotected sex. Do I still need emergency contraception?
Probably not, if you've been taking your pill correctly and consistently. The pill itself is preventing pregnancy. Emergency contraception (like Plan B) is just a high dose of hormones similar to the pill. Taking it on top of your regular pill can cause major hormonal disruption and nasty side effects like severe nausea and irregular bleeding for weeks. The only time to consider it is if you missed multiple active pills earlier in the pack or had severe vomiting/diarrhea that could have compromised your pill's effectiveness. When unsure, call your pharmacist or doctor—don't guess.
Can I use the pill to skip my period for a vacation or special event?
Absolutely. This is one of the great benefits. Simply skip the placebo pills (the inactive pills at the end of the pack) and start a new pack of active pills immediately. You might experience some breakthrough spotting, but you likely won't get a full period. It's perfectly safe to do this occasionally or even continuously, as endorsed by organizations like the American College of Obstetricians and Gynecologists. Some brands are even designed for this with 84 active pills followed by 7 placebos.
My friend had a terrible experience with one pill brand, but my doctor prescribed it to me. Should I be worried?
Not necessarily. Reactions are highly individual. The progestin type, estrogen dose, and even the inactive fillers in the pill can affect people differently. Your friend's nightmare might be your perfect match, and vice versa. Use her experience as a data point, not a verdict. Start the pill, monitor your own body closely for the first 3 months, and keep a simple journal of any symptoms. That's your best evidence.
The birth control pill is a tool. Like any tool, it works best when you understand how to use it properly. It's not a magical solution without trade-offs, nor is it a dangerous drug to be feared irrationally. It's a medical option that gives millions of women control over their reproductive health and cycles. Have an open, detailed conversation with your healthcare provider. Be your own advocate. Know that finding the right fit might take a cycle or two, but the clarity and control can be well worth it.




Leave a comment