Let's be honest: when it comes to health, women often put others first. But ignoring diabetes risks? That's a mistake I've seen too many times in my years as a healthcare consultant. Diabetes doesn't always shout; sometimes it whispers, especially in women. You might feel tired, blame it on stress, and move on. But what if it's more? Testing for diabetes isn't just about pricking your finger—it's about understanding your body's signals and taking control. In this guide, I'll walk you through exactly how to test for diabetes in women, based on real-world experience and avoiding the common pitfalls most articles gloss over.
Jump to What Matters
- Why Diabetes Testing is Non-Negotiable for Women
- How to Test for Diabetes: The 3 Main Methods Explained
- Step-by-Step Guide to Getting Tested
- Understanding Your Test Results: What the Numbers Really Mean
- Special Considerations for Women: Beyond the Basics
- Prevention and Management: Actionable Tips
- Your Questions Answered: FAQ Section
Why Diabetes Testing is Non-Negotiable for Women
Diabetes in women isn't the same as in men. Hormonal changes, pregnancy, and even menopause can twist the plot. The Centers for Disease Control and Prevention (CDC) notes that women with diabetes face higher risks of heart disease and complications like urinary infections. But here's the kicker: many women dismiss early symptoms as "just part of being busy." I recall a client, Sarah, who thought her constant thirst was from her new workout routine. It wasn't—it was undiagnosed type 2 diabetes. She caught it late because she avoided testing, assuming it was for older adults.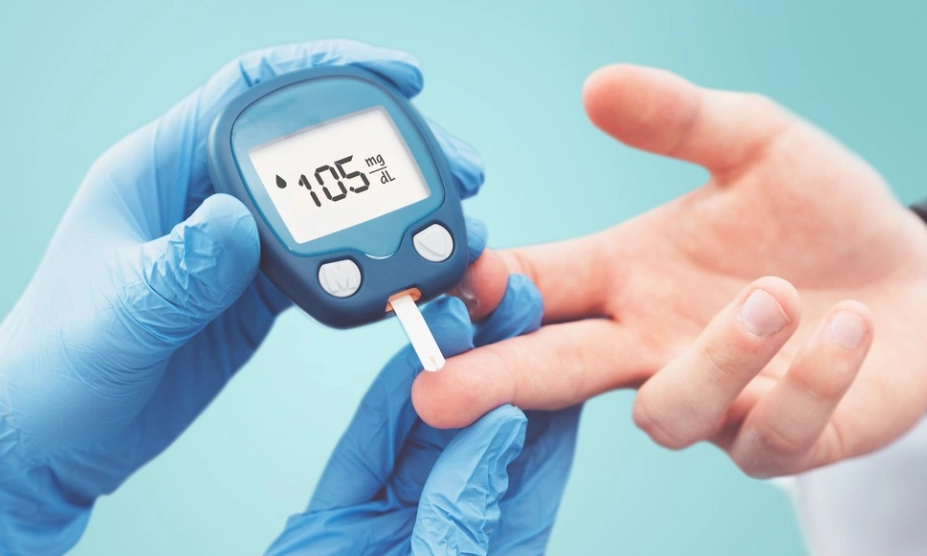
Women-specific risk factors include:
- Polycystic ovary syndrome (PCOS): Ups insulin resistance, doubling diabetes risk. A study in the Journal of Clinical Endocrinology & Metabolism highlights this link.
- Gestational diabetes: During pregnancy, it can vanish after birth but leaves a 50% chance of developing type 2 diabetes later. Most women don't get follow-up tests.
- Menopause: Hormonal shifts can spike blood sugar levels. It's a sneaky time when weight gain and fatigue mask deeper issues.
Testing early can prevent nerve damage, vision loss, and cardiovascular problems. Don't wait for symptoms to scream; get tested if you're over 45, overweight, or have a family history. For women under 45, consider testing if you have PCOS or had gestational diabetes.
How to Test for Diabetes: The 3 Main Methods Explained
There's no one-size-fits-all test. Doctors use a combo, but here are the core methods. I've seen patients confused by jargon, so let's break it down simply.
Fasting Blood Sugar Test
You fast for at least 8 hours (usually overnight), then get blood drawn at a clinic. It measures glucose levels in milligrams per deciliter (mg/dL). Normal is below 100 mg/dL; 100-125 mg/dL indicates prediabetes; 126 mg/dL or higher suggests diabetes. Cost? Around $50-$100 without insurance, but many clinics cover it. The catch: if you cheat on fasting, results skew. I've had clients drink juice thinking "it's just a sip," and it ruined the test.
A1C Test (Hemoglobin A1C)
This is my go-to for a broader picture. It averages blood sugar levels over the past 2-3 months, no fasting needed. Results are in percentages: under 5.7% is normal, 5.7%-6.4% is prediabetes, 6.5% or higher means diabetes. The American Diabetes Association recommends it for diagnosis. But note: conditions like anemia can affect accuracy. A friend with iron deficiency got a false high reading once—her doctor had to double-check with another test.
Oral Glucose Tolerance Test (OGTT)
Used often for gestational diabetes. You fast, drink a sugary solution, and have blood drawn at intervals over 2 hours. It's more thorough but can be unpleasant—nausea is common. Levels above 140 mg/dL at 2 hours signal prediabetes; over 200 mg/dL indicates diabetes. For pregnant women, thresholds are lower. This test costs more, about $150-$200, but it's gold standard for catching subtle glucose spikes.
Quick Comparison: Which test is best? It depends. If you need a snapshot, go for fasting blood sugar. For long-term trends, A1C. For pregnancy or unclear cases, OGTT. Always consult a doctor to choose.
Step-by-Step Guide to Getting Tested
Don't just walk into a lab blindly. Here's a practical plan based on what I advise my clients.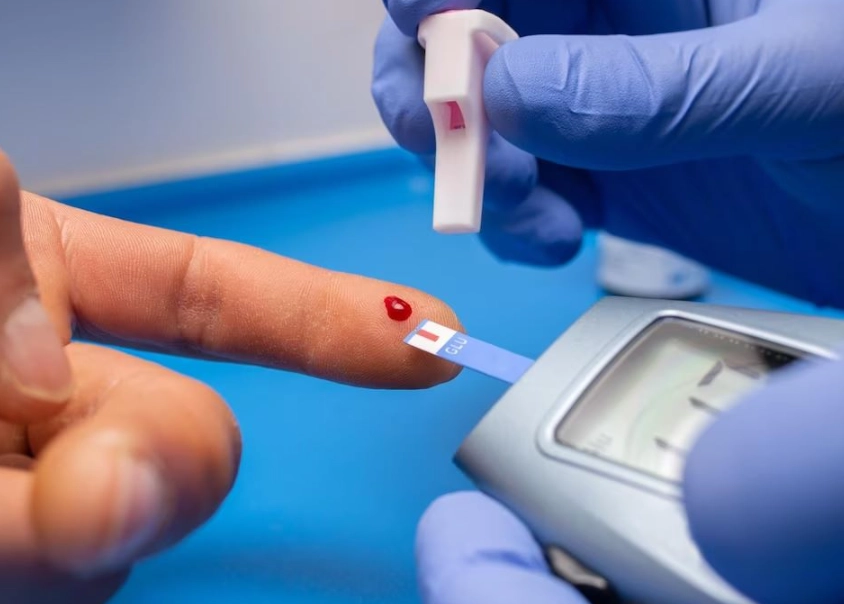
Step 1: Recognize Symptoms and Risks
List your symptoms: frequent urination, unexplained weight loss, blurred vision, fatigue. Note family history and personal factors like PCOS. Write them down—it helps at the doctor's office.
Step 2: Schedule a Doctor's Visit
Call your primary care physician or a clinic like Planned Parenthood for affordable options. Say, "I want to discuss diabetes testing due to [your symptoms/risks]." If you don't have a doctor, community health centers offer sliding-scale fees. Appointment wait times vary; book 2-3 weeks ahead.
Step 3: Prepare for the Test
For fasting tests: no food or drinks (except water) for 8-12 hours. Take medications as usual unless your doctor says otherwise. Wear loose sleeves for blood draws. Bring your ID and insurance card.
Step 4: Undergo the Test
At the lab, it's a quick blood draw—5-10 minutes. For OGTT, plan to stay 2 hours. Bring a book or podcast to pass time. If you're nervous, tell the technician; they're used to it.
Step 5: Get Results and Follow Up
Results come in 1-3 days. Don't panic if numbers are high. Schedule a follow-up to discuss next steps: lifestyle changes, medication, or further tests.
I remember helping a young mom, Maria, through this process. She was scared of needles, but we practiced deep breathing, and she got through it. Now, she tests annually and manages her prediabetes with diet.
Understanding Your Test Results: What the Numbers Really Mean
Numbers on a page can be confusing. Let's demystify them.
| Test Type | Normal Range | Prediabetes Range | Diabetes Range | What to Do Next |
|---|---|---|---|---|
| Fasting Blood Sugar | Below 100 mg/dL | 100-125 mg/dL | 126 mg/dL or higher | If prediabetes: lifestyle changes; if diabetes: see an endocrinologist. |
| A1C Test | Below 5.7% | 5.7%-6.4% | 6.5% or higher | Repeat test in 3-6 months if borderline; confirm with another method. |
| OGTT (2-hour) | Below 140 mg/dL | 140-199 mg/dL | 200 mg/dL or higher | For gestational diabetes: monitor diet; for others, consider medication. |
If your results are in the prediabetes range, don't ignore it. Many women think it's "not serious," but it's a red flag. A client of mine, Lisa, had an A1C of 6.0%. She switched to a low-carb diet and walked daily; in 6 months, it dropped to 5.5%. Action works.
For diabetes-range results, confirm with a second test on another day. False positives happen due to stress or illness. The World Health Organization advises confirmation for diagnosis.
Special Considerations for Women: Beyond the Basics
Women's bodies throw curveballs. Here's what most guides miss.
Pregnancy and Diabetes Testing
All pregnant women should get tested for gestational diabetes between 24-28 weeks. The OGTT is standard. But if you have risk factors like obesity or family history, test earlier. After birth, get tested at 6-12 weeks postpartum—many skip this, but it's crucial. I've seen women develop type 2 diabetes within a year because they assumed "it went away."
Menopause and Hormonal Fluctuations
During perimenopause, estrogen drops can increase insulin resistance. Test annually if you're over 50, even if you feel fine. Hormone replacement therapy might affect results; discuss with your doctor.
PCOS and Insulin Resistance
With PCOS, get tested yearly. Insulin levels might be high even if glucose is normal. Ask for a fasting insulin test alongside glucose tests—it's not routine but can reveal hidden issues.
Another nuance: menstrual cycles. Blood sugar can fluctuate with your cycle. Test at the same time each month for consistency. A study in Diabetes Care notes higher glucose levels in the luteal phase.
Prevention and Management: Actionable Tips
Testing is step one; prevention is key. Based on my experience, here's what works.
- Diet: Focus on fiber-rich foods—vegetables, whole grains. Cut added sugars. A Mediterranean diet has shown promise in reducing diabetes risk. Don't fall for fads; consistency matters.
- Exercise: Aim for 150 minutes of moderate activity weekly. Brisk walking counts. Strength training twice a week improves insulin sensitivity. I advise clients to start small—10-minute walks build habits.
- Weight Management: Losing 5-7% of body weight can slash diabetes risk by 58%. It's not about drastic diets; slow, steady loss works.
- Sleep and Stress: Poor sleep spikes cortisol, raising blood sugar. Aim for 7-8 hours. Try mindfulness or yoga—stress management is often overlooked.
For those with diabetes, monitoring is ongoing. Use a glucometer at home if advised. Continuous glucose monitors (CGMs) are a game-changer for some women, offering real-time data. They're pricey but worth it if you struggle with control.
Your Questions Answered: FAQ Section
Testing for diabetes in women isn't just a medical procedure; it's a step toward empowerment. By understanding the how and why, you can take charge of your health journey. Remember, numbers are tools, not verdicts. Start with a conversation with your doctor, and use this guide as your roadmap. Stay informed, stay proactive.




Leave a comment