If you're reading this, chances are you or someone you know is dealing with pelvic pain that just won't quit. Maybe it's cramps that knock you out every month, pain during sex, or a gut feeling that something's off. I've been a gynecologist for over a decade, and I've seen too many women struggle for years before getting an endometriosis diagnosis. Let's change that. This guide isn't just a list of steps—it's a roadmap based on real patient experiences and clinical insights.
What You'll Find in This Guide
Understanding Endometriosis Symptoms Beyond Pain
Endometriosis isn't just about bad periods. It's a whole-body condition where tissue similar to the uterine lining grows outside the uterus, causing inflammation, scarring, and a mess of symptoms. The classic signs include pelvic pain that cycles with your period, pain during or after sex, and heavy bleeding. But here's what many miss: fatigue, digestive issues like bloating or diarrhea around your period, and even pain with bowel movements.
I had a patient, Lisa, who came to me after five years of being told her pain was anxiety. She kept a symptom diary and noticed her pain spiked during ovulation, not just her period. That clue helped us pinpoint endometriosis. Stories like Lisa's are why tracking matters—symptoms can be sneaky.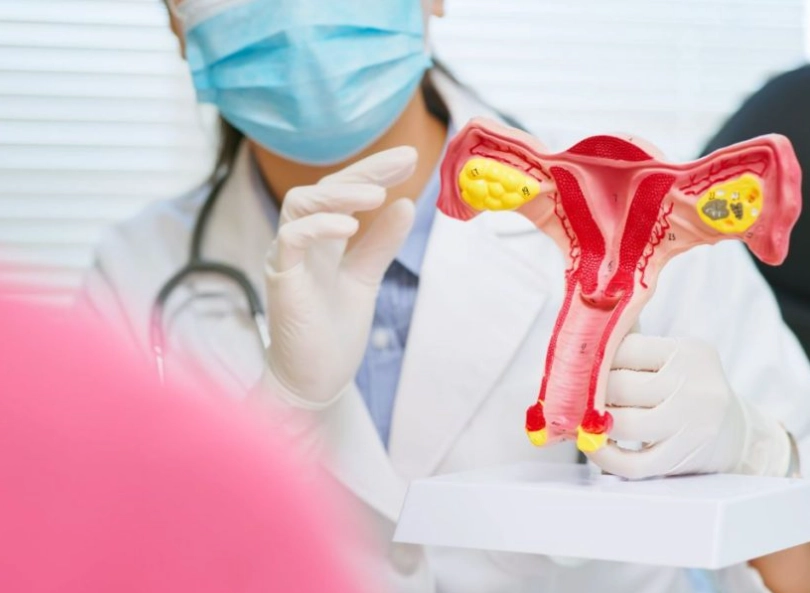
Common but overlooked symptoms: chronic lower back pain, urinary urgency during periods, and infertility without other obvious causes. If you have these, don't dismiss them.
The Diagnostic Journey: From Suspicion to Confirmation
Diagnosing endometriosis is a process, not a single test. It often starts with you noticing patterns in your body. From there, it's a collaborative effort with healthcare providers.
Step 1: Tracking Your Symptoms
Before you even see a doctor, start a symptom log. Use an app or a notebook. Note pain intensity (on a scale of 1-10), timing with your cycle, and any triggers like certain foods or activities. This data is powerful—it turns vague complaints into concrete evidence.
Step 2: The Initial Doctor's Visit
When you schedule an appointment, choose a gynecologist if possible. During the visit, expect a detailed history and a pelvic exam. The pelvic exam might reveal tenderness or nodules, but it's not definitive. Some doctors might press on specific areas to check for pain—this can hint at endometriosis, but it's not proof.
One mistake I see: patients downplaying their pain. Be honest. If it's a 8 out of 10, say so. Use your symptom log to back it up.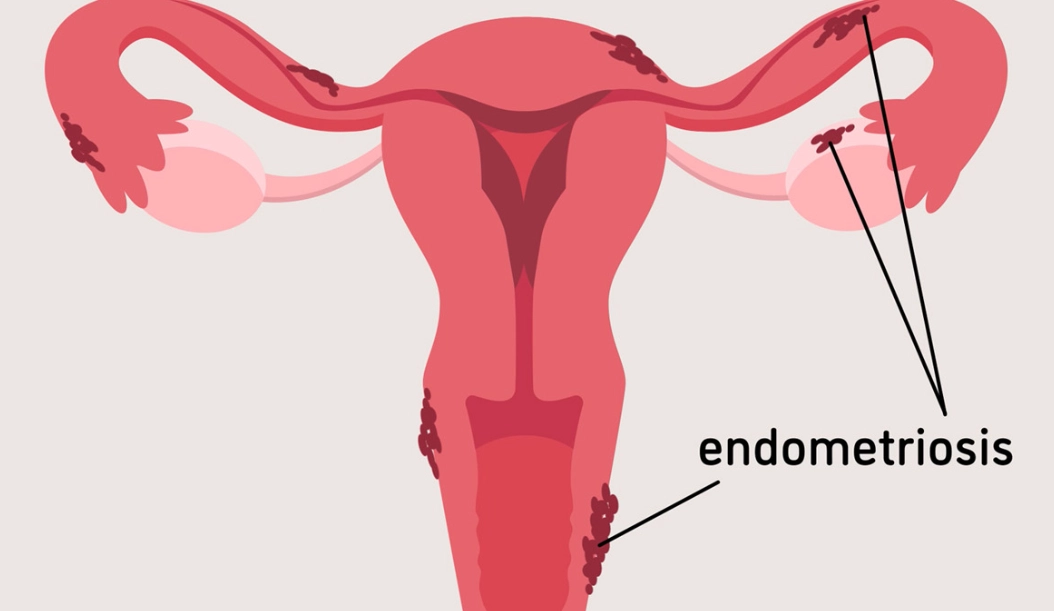
Key Diagnostic Tests for Endometriosis
After the initial evaluation, your doctor might order tests. Here's a breakdown of what each does and doesn't tell you.
Take Maria, a 28-year-old with severe pelvic pain. Her ultrasound was normal, but an MRI showed deep infiltrating endometriosis on her bowel. Without the MRI, she might have been told it was all in her head. Imaging isn't perfect, but in skilled hands, it can reveal a lot.
Ultrasound: The First Imaging Step
A transvaginal ultrasound is often the go-to. It's non-invasive and can detect ovarian endometriomas (chocolate cysts) or signs of deep disease. But here's the catch: a normal ultrasound doesn't rule out endometriosis. Superficial lesions are often invisible on ultrasound. According to the American College of Obstetricians and Gynecologists, ultrasound has limited sensitivity for early-stage disease.
MRI: For a Deeper Look
Magnetic resonance imaging (MRI) is more detailed. It's better at spotting deep infiltrating endometriosis, especially in areas like the rectum or bladder. However, it's more expensive and not always accessible. Insurance might require prior authorization.
In my practice, I recommend MRI when symptoms suggest deep disease or if ultrasound is inconclusive. But it's not a routine test for everyone.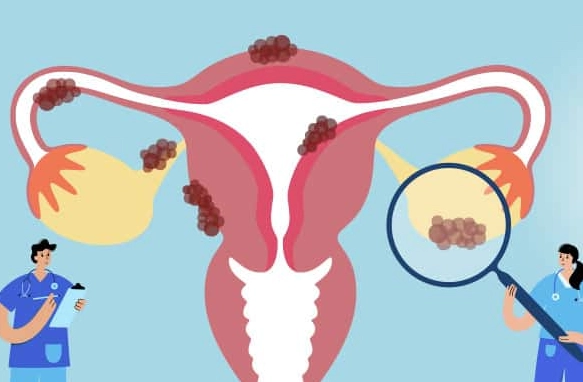
Other Tests: Blood Work and Beyond
There's no blood test that definitively diagnoses endometriosis. Some markers like CA-125 might be elevated, but they're non-specific—they can be high in other conditions like ovarian cancer or even during menstruation. Don't rely on blood tests alone.
Why Laparoscopy is Often the Gold Standard
Laparoscopy is a minimally invasive surgery where a surgeon inserts a camera through small incisions in the abdomen to visually inspect for endometriosis lesions. Biopsies can be taken to confirm the diagnosis. It's the only way to see the disease directly.
But surgery comes with risks: infection, bleeding, or anesthesia complications. The recovery time is usually a week or two. The upside? If endometriosis is found, it can often be treated during the same procedure—removing lesions can relieve symptoms.
A common misconception: laparoscopy is always necessary. Not true. For some patients, especially those with mild symptoms or who respond well to hormonal therapy, doctors might opt for a clinical diagnosis without surgery. But if symptoms persist or fertility is a concern, laparoscopy provides clarity.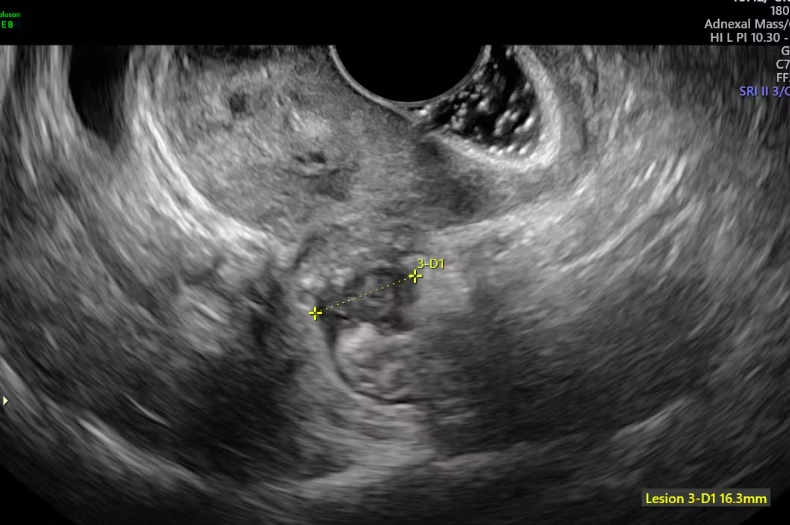
Navigating the Healthcare System: Tips from an Expert
The average delay in endometriosis diagnosis is 7-10 years. Why? Symptoms are normalized, and there's a lack of awareness. I've seen patients bounce between gastroenterologists, urologists, and gynecologists before getting answers.
My advice: be persistent. If your doctor dismisses you, seek a second opinion. Look for a specialist in endometriosis or pelvic pain—organizations like the Endometriosis Foundation of America have directories. Come to appointments prepared with your symptom log and a list of questions.
Questions to ask: 'What are the next steps if tests are normal?' 'Do you have experience with endometriosis surgery?' 'What are the risks and benefits of laparoscopy for me?'
Insurance can be a hurdle. Pre-authorization for tests or surgery might be needed. Keep records of all communications. If denied, appeal with supporting evidence from your doctor.




Leave a comment