Spotting the early signs of diabetes can feel like trying to solve a puzzle with pieces that don't quite fit. For women, the picture is often more complex. The symptoms can be subtle, easily blamed on a hectic life, stress, or just "getting older." But catching them early is a game-changer. It's the difference between managing a condition proactively and dealing with complications down the line. Let's cut through the noise and look at what really matters.
What You'll Find in This Guide
The Most Common Early Diabetes Signs (They're Not What You Think)
Forget the dramatic scenes from movies. Early diabetes whispers; it doesn't scream. The signs are often a collection of nagging, everyday issues that you might not connect. Here’s the breakdown.
Extreme fatigue and brain fog. This isn't just "I need a coffee" tired. It's a deep, persistent exhaustion that doesn't improve with sleep. You might feel like you're moving through mud by 2 PM. The brain fog is real too—forgetting words, losing your train of thought. It happens because your cells are starving for energy (glucose) that's stuck in your bloodstream.
Thirst and frequent urination. They go hand-in-hand. When blood sugar is high, your kidneys work overtime to filter it out, pulling extra water from your tissues. This makes you pee more (including waking up multiple times at night). Losing all that fluid makes you desperately thirsty. It’s a cycle.
Unexpected weight changes. This one trips people up. With type 1 diabetes, you might lose weight rapidly despite eating normally because your body starts burning fat and muscle for energy. With type 2, you might gain weight, especially around the abdomen, as insulin resistance worsens. Both are red flags.
Blurred vision. High blood sugar causes the lens in your eye to swell, changing its shape and focus. Your vision might get fuzzy, or you might have trouble focusing. It's usually temporary and improves with better blood sugar control, but ignoring it is a mistake.
Slow-healing cuts and frequent infections. High glucose impairs blood circulation and weakens your immune system's white blood cells. A small paper cut takes weeks to heal. You get more yeast infections, urinary tract infections (UTIs), or skin infections like boils.
| Symptom | More Common in Type 1 | More Common in Type 2 | Why It Happens |
|---|---|---|---|
| Sudden Weight Loss | Very Common | Less Common (Early) | Body burns fat/muscle for fuel |
| Increased Hunger | Very Common | Common | Cells aren't getting energy |
| Yeast Infections | Common | Very Common | Yeast thrives on high glucose |
| Acanthosis Nigricans (dark skin patches) | Rare | Common | Sign of insulin resistance |
Symptoms That Shout Louder in Women's Health
This is the part most general articles gloss over. Diabetes interacts directly with female reproductive hormones, creating a unique set of warning signs.
Polycystic Ovary Syndrome (PCOS) is a Major Clue
If you have PCOS, listen up. Insulin resistance is a core driver of PCOS. The Centers for Disease Control and Prevention (CDC) states that over half of women with PCOS develop type 2 diabetes by age 40. It's not just a coincidence; it's a direct pathway. Irregular periods, excess hair growth, and acne from PCOS can be early metabolic distress signals.
Vaginal and Urinary Issues
Recurrent yeast infections or bacterial vaginosis are classic. The sugar-rich environment in vaginal fluids is a paradise for yeast. Many women get stuck in a cycle of treatments without anyone checking their blood sugar. Similarly, frequent UTIs become a frustrating norm.
Then there's sexual health. Diabetes can damage small blood vessels and nerves, leading to decreased lubrication, discomfort during sex, and reduced sensation. It's a sensitive topic, but a significant one.
Pregnancy-Related Red Flags
A history of gestational diabetes is one of the strongest predictors for developing type 2 diabetes later. It's like your body did a "stress test" and showed it struggles with blood sugar under load. Also, having a baby weighing over 9 pounds at birth is another indicator.
For women going through menopause, fluctuating hormones can make blood sugar control even wilder, sometimes unmasking previously hidden diabetes.
Why These Symptoms Happen: The Blood Sugar Connection
It all boils down to insulin, a hormone that acts like a key. It unlocks your cells to let glucose (sugar) in from your blood for energy.
In type 1 diabetes, your immune system destroys the cells that make insulin. No key, no entry. Glucose piles up in your blood, causing the symptoms.
In type 2 diabetes, your cells become resistant to insulin (the lock gets rusty). Your pancreas makes more and more keys to try and force it open, but eventually it burns out. Again, glucose builds up.
That excess blood glucose is toxic. It's like spilling syrup in your bloodstream—it gums up the works. It damages nerves (causing numbness, tingling), small blood vessels (affecting eyes, kidneys, healing), and large vessels (increasing heart disease risk). The symptoms we discussed are your body's alarm system for this internal spill.
What to Do If You Recognize These Signs
Don't panic. But do act. Ignoring it won't make it go away.
Step 1: Schedule a doctor's appointment. Don't downplay your symptoms. Say, "I'm experiencing X, Y, and Z, and I'm concerned about my blood sugar." Be specific. Write down your symptoms and when they started before you go.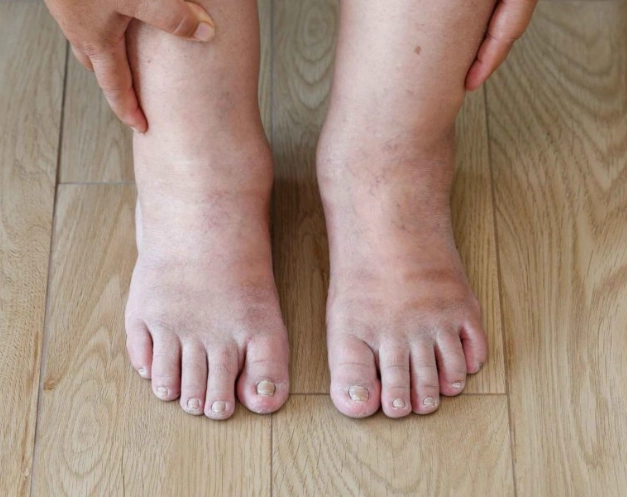
Step 2: Know the tests. Your doctor will likely order one of these:
- Fasting Plasma Glucose (FPG): Blood test after not eating for 8+ hours.
- Hemoglobin A1c (HbA1c): Your average blood sugar over the past 2-3 months. This is the gold standard.
- Oral Glucose Tolerance Test (OGTT): Drink a sugary liquid, then test blood over 2 hours.
Step 3: Start observing now. Notice how you feel after eating a carb-heavy meal (pasta, bread, sweets). Do you crash an hour later? Feel incredibly thirsty? This self-awareness is powerful data for you and your doctor.
Let me tell you about Sarah, a former client. She was 42, constantly tired, battling yeast infections, and couldn't lose weight despite rigorous exercise. She thought it was perimenopause. Her doctor initially agreed. It was only when she specifically asked for an A1c test that they found her level at 6.8% (prediabetes range). That test, and her advocacy, started her on a path to reversal through diet and lifestyle changes. She didn't have to wait for full-blown diabetes.
Your Questions, Answered Honestly
If my symptoms come and go, does that mean it's not diabetes?
Not at all. Blood sugar levels fluctuate. You might feel fine on days you eat better or are less stressed, and worse on other days. The trend is what matters. Intermittent symptoms are common, especially in early type 2 diabetes or prediabetes. They're a sign your body is struggling to maintain balance, not proof that everything is okay.
I'm not overweight. Could I still have type 2 diabetes?
Absolutely. This is a huge misconception. While weight is a risk factor, thin people can and do develop insulin resistance and type 2 diabetes. It's called "lean diabetes" or "normal-weight diabetes." Genetics, poor diet (even if calories are low), lack of muscle mass, and chronic stress are major players. Don't let your weight rule out the possibility.
Are home blood glucose monitors useful for checking?
They can be a helpful screening tool, but with a major caveat. A single reading tells you very little. If you use one, check at different times: first thing in the morning (fasting) and 1-2 hours after a meal. Track the numbers for a week. Consistently high fasting readings (over 100 mg/dL or 5.6 mmol/L) or post-meal spikes (over 140 mg/dL or 7.8 mmol/L) warrant a doctor's visit. Remember, the A1c test is what gives the full picture.
What's the biggest mistake people make when they notice these signs?
Self-diagnosing with something else. "It's just stress." "I'm getting older." "I need more sleep." While those things can cause similar feelings, the combination of symptoms—especially thirst, frequent urination, and fatigue—is specific. The second mistake is being afraid of the diagnosis. Knowing is power. Prediabetes and early type 2 diabetes are often reversible with lifestyle changes. The longer you wait, the harder it becomes.
The bottom line? Your body has a sophisticated language of symptoms. The early signs of diabetes in women are its way of sending an urgent memo. Don't file it away. Listen, investigate, and take action. It's the most important health decision you can make for your future self.



Leave a comment