You've been trying for a while. Maybe it's been six months, a year, or longer. The negative tests, the tracking, the hope each month followed by disappointment—it's exhausting. The first thing you need to know is this: you're not alone. Infertility affects about 1 in 6 couples globally, according to the World Health Organization. And here's the crucial part many people miss: infertility is almost equally a male and female issue. Roughly one-third of cases are due to female factors, one-third to male factors, and one-third are a combination of both or unexplained. So, tackling it means looking at both partners from the start. This isn't a blame game; it's a team effort.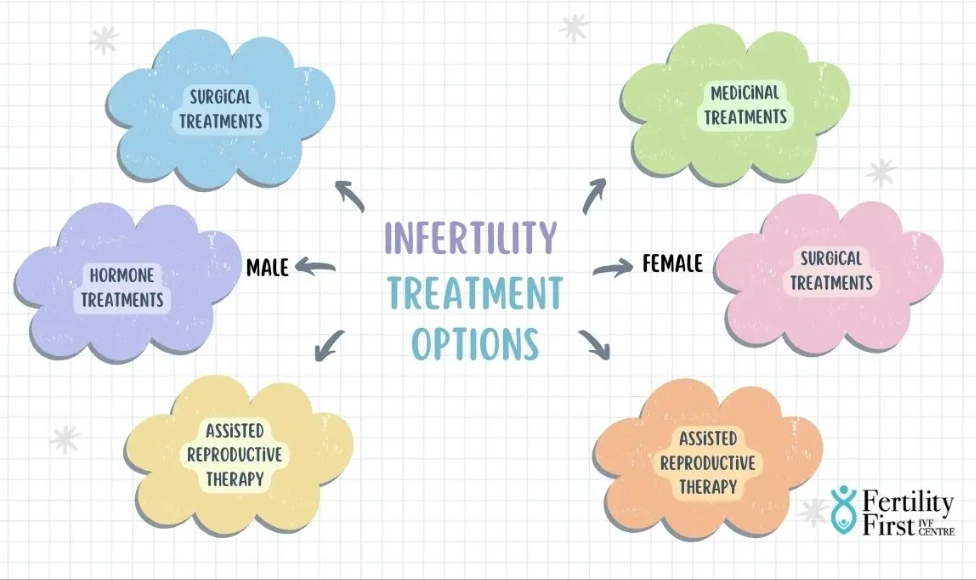
What’s Inside This Guide
I've worked with hundreds of couples over the years, and the most common mistake I see is rushing into treatment before a complete diagnosis. It's like trying to fix a car without knowing if the problem is the battery, the engine, or a flat tire. You'll waste time, money, and emotional energy. Let's break down the process logically.
How is Infertility Diagnosed for Both Partners?
Diagnosis is a dual-track process. A good fertility clinic will insist on evaluating both of you simultaneously. Don't let any doctor tell you to "just relax" or focus on one partner until the other is cleared.
For Men: The Semen Analysis (And Beyond)
The starting point is a semen analysis. This isn't just about sperm count. A comprehensive analysis looks at three key parameters, often called the "sperm trifecta":
- Count: How many sperm are there? (Normal is >15 million per milliliter).
- Motility: How well do they swim? (At least 40% should be moving).
- Morphology: What's their shape? (At least 4% should be normally formed).
But here's a subtle point many clinics overlook: a standard semen analysis doesn't check for sperm DNA fragmentation. You can have great numbers on paper, but if the sperm's genetic material is damaged, it can cause failed fertilization, poor embryo development, or miscarriage. If you've had multiple IVF failures or miscarriages, ask about this test specifically.
For Women: Tracking the Cycle
The female fertility workup is more complex because it involves multiple systems. Key tests include:
- Ovulation Tracking: Confirming you're releasing an egg. This can involve at-home ovulation predictor kits, blood tests for progesterone, or transvaginal ultrasounds.
- Hormone Panel: Blood tests for FSH, LH, AMH, estradiol, and thyroid function. AMH gives a rough idea of your ovarian reserve (egg supply).
- Hysterosalpingogram (HSG): An X-ray test to check if your fallopian tubes are open and the uterine cavity is normal. It's uncomfortable but quick.
- Transvaginal Ultrasound: To look at the ovaries for cysts, count antral follicles (another reserve marker), and examine the uterus for fibroids or polyps.
What are the Treatment Options for Male Infertility?
Gone are the days when male infertility meant a dead end. There are now more solutions than ever, ranging from lifestyle changes to advanced surgical sperm retrieval.
| Treatment | Best For | What It Involves | Approx. Cost (USD) |
|---|---|---|---|
| Lifestyle & Medication | Hormonal imbalances, mild sperm issues, varicoceles. | Quitting smoking, reducing alcohol, managing weight. Medications like Clomid (clomiphene) to boost testosterone/sperm production. Surgery to repair a varicocele (enlarged vein in the scrotum). | $500 - $5,000+ (for surgery) |
| Intrauterine Insemination (IUI) with Washed Sperm | Mild to moderate male factor (low count/motility), unexplained infertility. | Semen sample is "washed" in the lab to concentrate the healthiest, most motile sperm. These are then placed directly into the uterus around ovulation, bypassing the cervix. | $300 - $1,000 per cycle |
| In Vitro Fertilization (IVF) with ICSI | Severe male factor (very low count, poor motility, high DNA fragmentation), previous IUI failures. | IVF retrieves eggs from the woman. Then, a single sperm is injected directly into each mature egg (ICSI). This is the gold standard for severe male factor infertility. | $12,000 - $20,000+ per cycle |
| Surgical Sperm Retrieval (TESA/PESA) | Obstructive azoospermia (no sperm in ejaculate due to blockage) or failed vasectomy reversal. | Minor procedures to extract sperm directly from the testicle (TESA) or epididymis (PESA). The retrieved sperm is then used for ICSI. | $2,000 - $6,000 + IVF/ICSI costs |
A personal observation: the obsession with "count" often overshadows the importance of sperm health. I've seen couples spend years on supplements for a modest count increase, while ignoring high DNA fragmentation that was the real barrier. If you're going the IVF route, ask your lab about using PICSI or IMSI—advanced sperm selection techniques that can improve outcomes for some men.
What are the Treatment Options for Female Infertility?
Treatment depends entirely on the diagnosed cause. It's not one-size-fits-all.
Ovulation Disorders (like PCOS)
This is one of the most common and treatable causes. The first-line treatment is usually oral medications:
- Clomiphene Citrate (Clomid) or Letrozole (Femara): These stimulate the ovaries to develop and release eggs. Letrozole is often preferred for women with PCOS as it may have a lower risk of multiple births and thin uterine lining.
- Metformin: Used for insulin resistance often associated with PCOS.
- Gonadotropin Injections: Stronger, injectable hormones used if oral meds fail. They require close monitoring via ultrasound to avoid ovarian hyperstimulation syndrome (OHSS).
Tubal or Uterine Issues
If the fallopian tubes are blocked or damaged, surgery might be an option for mild cases, but success rates vary. Often, IVF is the recommended path because it completely bypasses the tubes. For uterine issues like fibroids or polyps, a hysteroscopic surgery can often remove them, improving the chances for both natural conception and IVF.
Endometriosis
This can cause inflammation and scarring. Laparoscopic surgery to remove endometrial implants can improve fertility. However, for moderate to severe cases, or if surgery doesn't lead to pregnancy within 6-12 months, moving to IVF is common.
Diminished Ovarian Reserve (DOR) or Age-Related Fertility Decline
This is the toughest one, because you can't make more eggs. The focus shifts to working with the eggs you have as efficiently as possible. IVF with aggressive stimulation protocols is typically the main option. Using donor eggs becomes a very real and often successful conversation for women with very low reserve.
Let me paint a scenario. Sarah, 34, has PCOS and isn't ovulating regularly. Her husband, Mark, has a slightly low sperm count. They start with 3 cycles of Letrozole + timed intercourse. No luck. They move to 3 cycles of Letrozole + IUI. Still nothing. At this point, they're frustrated. The diagnosis? Combined factors. Sarah's PCOS and Mark's borderline sperm create a cumulative hurdle. They move to IVF with ICSI, which addresses both issues simultaneously—controlling Sarah's ovulation in a lab setting and selecting Mark's best sperm for injection. It worked on their first IVF cycle.
Understanding Assisted Reproductive Technology (ART): IUI vs. IVF
These are the two main assisted reproduction procedures. People get confused about the difference.
Intrauterine Insemination (IUI) is like giving the sperm a head start. It's a relatively simple, in-office procedure. It's best for:
- Unexplained infertility.
- Mild male factor.
- Cervical factor issues.
- When using donor sperm.
Success rates per cycle are modest, typically 10-20%, depending on age and diagnosis. It's less invasive and cheaper than IVF, so it's often a logical first step if the tubes are open and sperm parameters are decent.
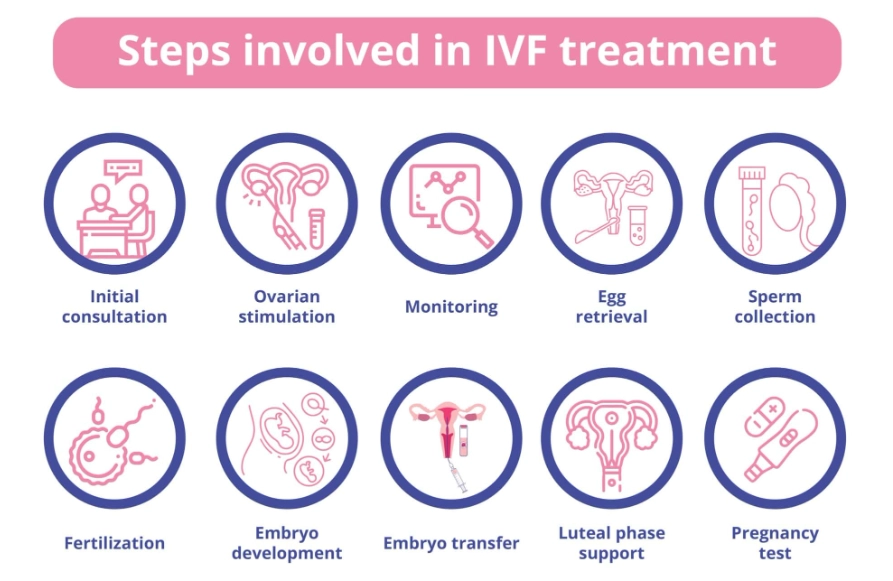
In Vitro Fertilization (IVF) is a full laboratory process. Eggs are retrieved, fertilized with sperm in a dish, embryos grow for 3-5 days, and then one (or sometimes two) are transferred to the uterus. ICSI (intracytoplasmic sperm injection) is often part of the process. IVF is for:
- Blocked or damaged fallopian tubes.
- Severe male factor infertility.
- Endometriosis.
- Advanced maternal age.
- Failed IUI cycles.
- Genetic screening needs (PGT-A).
Success rates are higher per cycle (often 40-60% for women under 35 for a single embryo transfer), but it's physically, emotionally, and financially intensive.
How to Choose the Right Infertility Treatment Path
This decision is personal. There's no single right answer. You need to weigh a four-sided scale:
- Medical Factors: What does your diagnosis dictate? Severe tubal damage means IVF. Very low sperm count likely means IVF with ICSI. This is the most objective factor.
- Financial Realities: Be brutally honest about your budget. IUI costs less per cycle but may require multiple cycles. IVF has a higher upfront cost but a higher per-cycle success rate. Check your insurance coverage meticulously.
- Emotional & Physical Bandwidth: IVF is a marathon. The daily injections, frequent monitoring appointments, and hormonal rollercoaster are real. Some couples prefer to try less invasive options first, even if the odds are lower, to avoid that strain.
- Time (Age): This is the non-negotiable. If the female partner is over 37, the decline in egg quality and quantity accelerates. In this case, spending a year on low-odds treatments like IUI might cost you more in terms of success rates than moving to IVF sooner. Don't let a doctor waste your time with protocols that have slim chances based on your age.
Have a frank conversation with your doctor. Ask: "Based on our combined diagnosis and my age, what is the realistic chance of success per cycle with IUI vs. IVF?" Get the numbers. Then make your choice.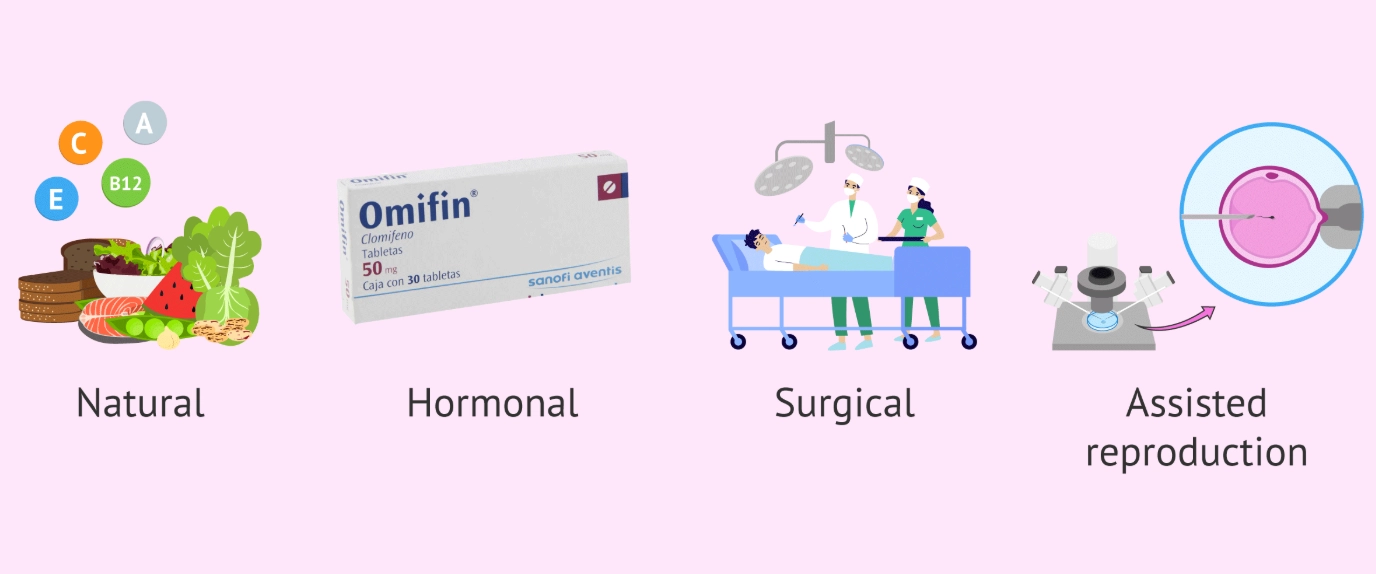
Your Burning Questions Answered
 The path through infertility treatment is rarely straight. It has detours, setbacks, and unexpected turns. But by understanding the causes, knowing all your options, and making informed decisions as a team, you can navigate it. Start with a thorough dual diagnosis, be realistic about the odds of each treatment tier, and don't be afraid to ask your doctor tough questions. Your journey is unique, but you have more tools and knowledge at your disposal than ever before.
The path through infertility treatment is rarely straight. It has detours, setbacks, and unexpected turns. But by understanding the causes, knowing all your options, and making informed decisions as a team, you can navigate it. Start with a thorough dual diagnosis, be realistic about the odds of each treatment tier, and don't be afraid to ask your doctor tough questions. Your journey is unique, but you have more tools and knowledge at your disposal than ever before.





Leave a comment