You feel off. Maybe it's the constant thirst, the trips to the bathroom that wake you up at night, or a fatigue that coffee just can't touch. You might brush it off as stress, getting older, or just a rough patch. But a quiet voice asks: could it be something more? For millions of women, that "something" is diabetes, and it often whispers before it shouts.
The tricky part? Many early diabetes symptoms in women are subtle, easily mistaken for other issues, or even dismissed as "just part of being a woman." I've seen it with friends and clients—smart, health-conscious women who missed the signs for years because they didn't know what to look for. The good news is, you don't have to guess. Knowing what to watch for and when to act is your most powerful tool.
What's Inside: Your Quick Guide
What Are the Key Symptoms of Diabetes in Women?
Let's move past the textbook list. Yes, the classic signs—excessive thirst, frequent urination, unexplained weight loss—apply. But in women, the story often has extra chapters. Your body might signal trouble in areas your doctor doesn't automatically connect to blood sugar.
The "Below the Belt" Signals Many Doctors Don't Ask About
High blood sugar creates an ideal environment for yeast and bacteria. This means recurrent, stubborn yeast infections or urinary tract infections (UTIs) can be a major red flag. If you're finding yourself needing treatment for these issues several times a year, it's not just bad luck. It's a sign your internal environment is out of balance.
Another rarely discussed symptom is sexual dysfunction. This isn't just about low libido. Diabetes can damage small blood vessels and nerves, leading to vaginal dryness, discomfort during sex, or difficulty achieving orgasm. It's embarrassing to bring up, so many women suffer in silence, never linking it to their metabolism.
A Real-Life Snapshot: My friend Sarah (name changed) spent two years battling constant fatigue and monthly yeast infections. Her gynecologist treated the infections but never suggested a blood sugar check. It was only when she mentioned her unquenchable thirst to a new primary care doctor that the dots were connected. Her HbA1c was in the diabetic range. She told me, "I thought I was just run down from work and being a mom. I had no idea my body was trying to tell me something so specific."
The Energy and Mood Rollercoaster
Fatigue is a huge one. Not the "I need a nap" kind, but a deep, bone-weary exhaustion that doesn't improve with rest. This happens because your cells are starving for energy (glucose) that's stuck in your bloodstream, unable to get in without enough insulin.
Then there's the mood connection. Irritability, anxiety, or feeling "hangry" are not just personality quirks. When blood sugar swings from high to low, it directly impacts your brain chemistry. You might find yourself snapping at loved ones or feeling unusually anxious for no clear reason.
Skin and Hair Changes You Might Blame on Aging
Look at your skin. Dark, velvety patches in body folds like your neck, armpits, or groin (a condition called acanthosis nigricans) are a direct sign of insulin resistance, the precursor to type 2 diabetes. It's often mistaken for a hygiene issue or just "darker skin."
Slow-healing cuts or bruises, especially on your legs and feet, are another clue. Your body's repair systems struggle when flooded with sugar. Thinning hair or hair loss on the scalp, coupled with increased facial hair, can also be related to the hormonal imbalances that accompany insulin problems and conditions like PCOS.
Why Are Women at Unique Risk for Diabetes?
It's not just lifestyle. Biology plays a starring role. Hormonal fluctuations throughout a woman's life directly interact with insulin sensitivity.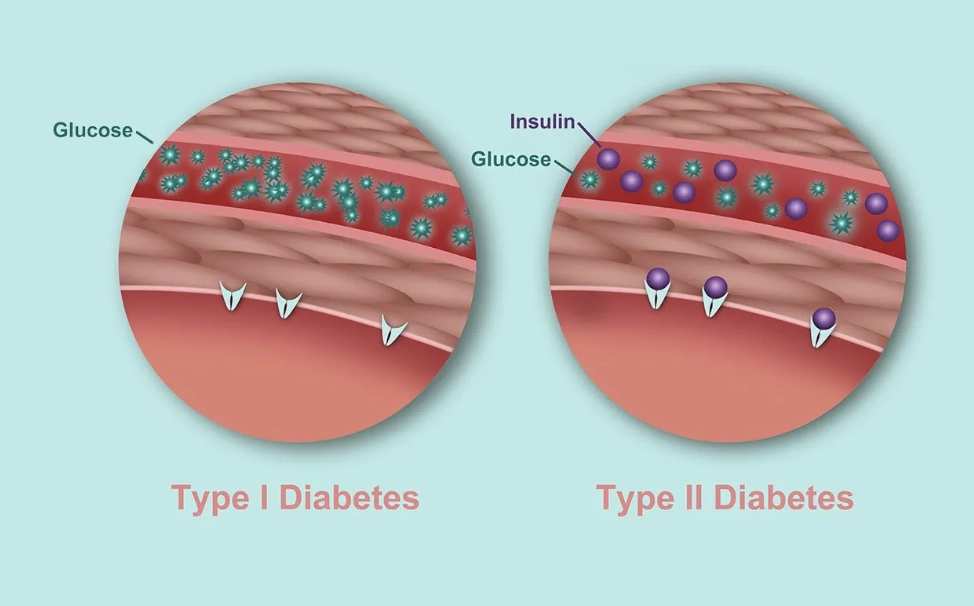
Polycystic Ovary Syndrome (PCOS): This is a massive, under-discussed link. Up to 70% of women with PCOS have insulin resistance. If you have irregular periods, acne, and excess hair growth, your diabetes risk is significantly higher, regardless of your weight. Treating PCOS often involves managing insulin first.
Pregnancy - A Metabolic Stress Test: Gestational diabetes is a glaring warning sign. It means your pancreas struggled to keep up with the insulin demand during pregnancy. While it often goes away after birth, it leaves a permanent mark. According to the Centers for Disease Control and Prevention (CDC), about 50% of women with gestational diabetes go on to develop type 2 diabetes later in life. It's not a one-time event; it's a preview.
Menopause: The drop in estrogen during menopause can increase abdominal fat and decrease insulin sensitivity. Many women see their blood sugar creep up for the first time in their late 40s and 50s, blaming weight gain on "slowing metabolism" when it's a specific hormonal shift.
The Silent Period: Here's a crucial point most articles miss: prediabetes often has no clear symptoms. You could walk around for years with elevated blood sugar damaging your blood vessels, feeling perfectly fine. That's why knowing your risk factors—family history, PCOS, past gestational diabetes, being over 45—is more important than waiting for symptoms. Waiting for a symptom is waiting too long.
How is Diabetes Officially Diagnosed? (It's Easier Than You Think)
Forget the old, awful sugar-drink tests you've heard about. Modern diagnosis is straightforward. You don't need dramatic symptoms to qualify for testing. If you have risk factors, that's reason enough.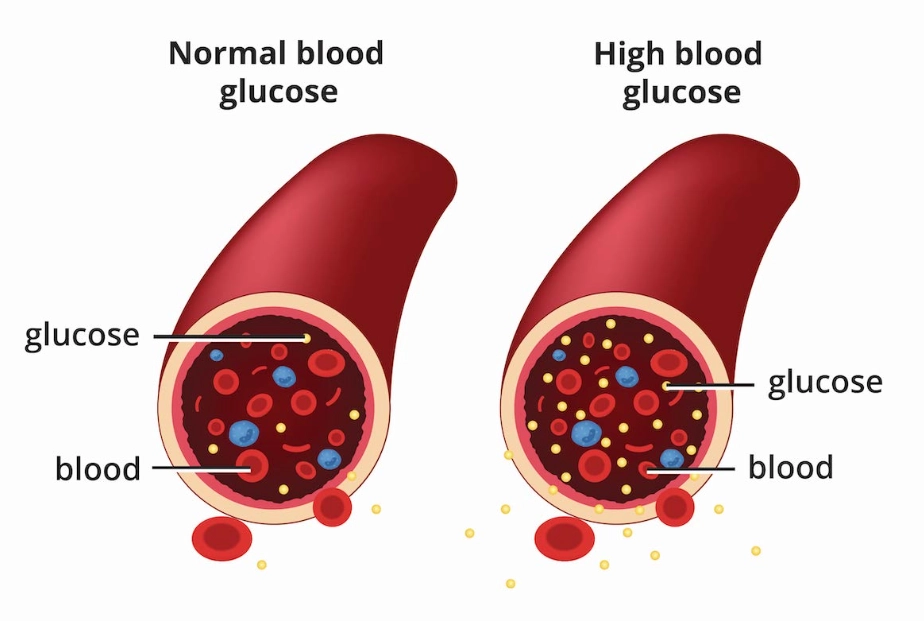
Here’s what your doctor can do:
1. The HbA1c Test (The 3-Month Report Card): This is the gold standard. A simple blood draw measures the percentage of your red blood cells that have sugar attached to them. It gives an average of your blood sugar levels over the past 2-3 months. No fasting needed.
- Normal: Below 5.7%
- Prediabetes: 5.7% to 6.4%
- Diabetes: 6.5% or higher
2. Fasting Plasma Glucose Test: You fast overnight (at least 8 hours), then get your blood drawn.
- Normal: Less than 100 mg/dL
- Prediabetes: 100 to 125 mg/dL
- Diabetes: 126 mg/dL or higher
3. Oral Glucose Tolerance Test (OGTT): This is less common now but used for diagnosing gestational diabetes. You fast, get a baseline blood draw, drink a sugary liquid, and have your blood tested again after 2 hours. A 2-hour level of 200 mg/dL or higher indicates diabetes.
The key is this: you only need one abnormal test result to be diagnosed with prediabetes or diabetes. Your doctor will likely repeat it to confirm, but don't let a single high number be dismissed as a "fluke."
I Think I Might Have Symptoms. What's My First Move?
Don't panic. Don't self-diagnose with a pharmacy glucometer (those are for management, not diagnosis). Your action plan is simple.
Step 1: Make the Appointment. Call your primary care doctor or an endocrinologist. Be direct. Say, "I'm concerned about my risk for diabetes because I have [mention your symptoms: constant fatigue, recurrent yeast infections, family history, past gestational diabetes]. I'd like to get my blood sugar checked." This frames it as a legitimate medical request, not just a vague worry.
Step 2: Track Your Observations. For a week before your appointment, jot down notes. When do you feel thirstiest? How often are you urinating? Note your energy crashes. This concrete data helps your doctor more than saying "I feel tired sometimes."
Step 3: Get the Right Tests. Ask specifically for an HbA1c test. It's the most informative single test. A fasting glucose test is also a good start. If you have symptoms of PCOS, ask for hormone panels as well.
Step 4: Understand the Numbers. Ask for a copy of your results and have your doctor explain what every value means. "Normal" on the lab report has a range. Where do you sit in that range? An A1c of 5.6% is technically normal but knocking on prediabetes's door.
The goal isn't to find a problem. The goal is to get information. Information is power. Whether the result is normal, shows prediabetes, or diabetes, you now have a clear starting point to take control of your health.
Your Questions, Answered
I have some symptoms, but I lost a few pounds and they got better. Do I still need testing?
My doctor said my fasting sugar is "a little high" but not diabetic, and to just watch my diet. Is that enough?
Can diabetes be reversed if I catch it early?
Are the symptoms different for Type 1 vs. Type 2 diabetes in women?
I'm scared of getting a diagnosis. Isn't ignorance bliss?





Leave a comment