Let's cut to the chase. You've been trying to conceive. Maybe it's been six months, maybe a year, maybe longer. That hopeful feeling each month is starting to mix with a quiet, nagging worry. "Is something wrong?" "How would I even know?" The uncertainty itself is exhausting. The truth is, fertility issues often whisper before they shout. They show up in subtle signs your body gives you, long before a doctor makes an official diagnosis. This isn't about fear-mongering; it's about awareness. Knowing these signs empowers you to take action sooner, which is often the single biggest factor in a positive outcome.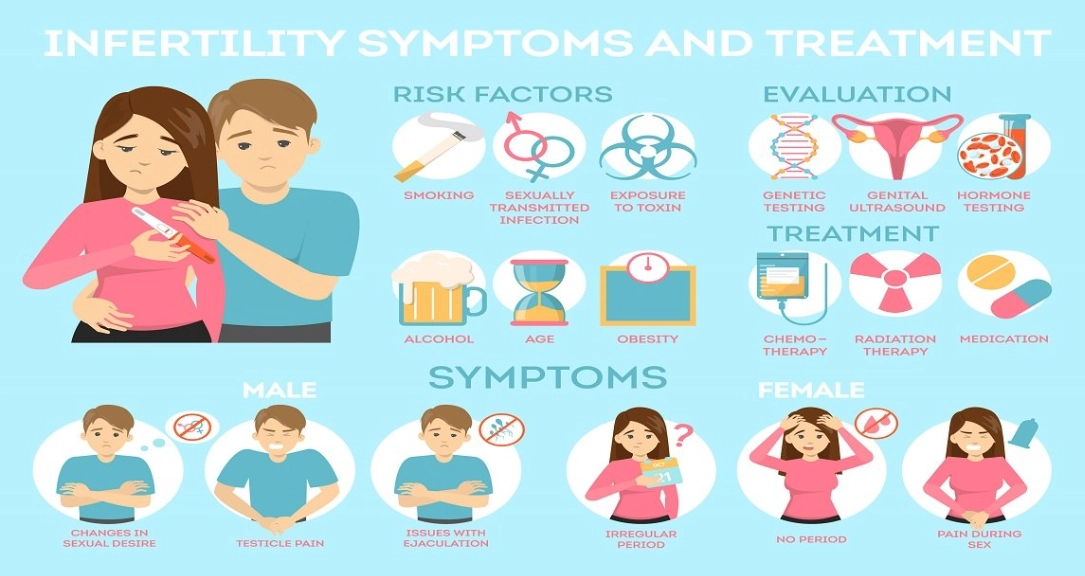
Quick Navigation: What's in This Guide
7 Key Signs That Might Indicate a Fertility Problem
Forget the vague advice. Here are the concrete, physical and situational clues that suggest it's time to look deeper. I've seen too many people dismiss these for years, thinking it's just "bad luck."
1. Irregular or Absent Menstrual Cycles
This is the big one. A cycle that's consistently shorter than 21 days or longer than 35 days isn't just inconvenient—it's a red flag for potential ovulation disorders. No period (amenorrhea) for several months when you're not pregnant is a clear signal your reproductive system isn't cycling normally. Polycystic Ovary Syndrome (PCOS) is a common culprit here, affecting up to 1 in 10 women of childbearing age according to the Office on Women's Health.
2. Painful Periods or Pain During Sex
Bad cramps are common, but debilitating pain that interferes with your life isn't normal. Similarly, deep pain during intercourse can be a symptom of endometriosis or pelvic inflammatory disease (PID). These conditions cause inflammation and scarring that can directly block fallopian tubes or impair egg quality. A lot of women are told to just "put up with it," but that pain is information. Listen to it.
Personal Note: I worked with a client who had painful periods for 15 years, assuming it was just her lot in life. It wasn't until she struggled to conceive that an MRI revealed stage IV endometriosis. Addressing the pain earlier could have preserved more of her fertility.
3. You've Been Trying for Over a Year (or 6 Months if You're Over 35)
This is the clinical definition of infertility. About 85% of couples will conceive within a year of regular, unprotected sex. If you haven't, it's not a judgment, it's a statistical indicator that something might need investigation. For women over 35, the timeline shortens to 6 months because time becomes a more critical factor with egg quality.
4. A History of Miscarriages
Two or more consecutive pregnancy losses are considered recurrent miscarriage and warrant a fertility workup. It suggests the body is getting pregnant but unable to sustain it, which points to potential issues with egg/sperm quality, uterine structure, or immune factors.
5. Known Hormonal Issues
Conditions like thyroid disorders (both overactive and underactive), uncontrolled diabetes, or high prolactin levels can throw your entire reproductive hormone orchestra out of tune. Symptoms like unexplained weight changes, severe acne, excessive facial hair, or thinning scalp hair can be external signs of these internal hormonal imbalances.
6. For Men: Changes in Sexual Function or Testicular Issues
Fertility isn't a "woman's problem." Male factors contribute to about 30-40% of cases. Signs include problems with erection or ejaculation, pain or swelling in the testicles, a history of trauma or surgery in the groin area, or a low sex drive. Even if none of these are present, a low sperm count has no obvious symptoms—which is why male testing is a non-negotiable first step.
7. A Gut Feeling That Something Isn't Right
This sounds vague, but I trust it. You know your body better than anyone. If you have a persistent intuition that your cycles are "off," or that conception feels inexplicably difficult despite timing everything right, that's valid data. Don't let anyone dismiss it as anxiety. It's often the catalyst for finding a real, underlying issue.
What to Do If You Suspect a Fertility Problem
Don't panic. Suspecting a problem is the first step toward solving it. Here’s a practical, step-by-step action plan.
Step 1: Start Tracking (Really Tracking)
Go beyond an app that just predicts. For 2-3 cycles, track basal body temperature (BBT) every morning and observe cervical mucus changes. This isn't just for timing sex; it's hard data for your doctor. A BBT chart that doesn't show a clear temperature shift can be proof you're not ovulating. I recommend the methods taught by FertilityFriend or taking a course from a certified instructor.
Step 2: Schedule a Preconception Checkup
See your OB/GYN or a primary care doctor. Come with your cycle charts and a list of your concerns. Be blunt. Say, "We've been trying for X months, and I'm worried because of Y symptom. What tests can we do?" A basic check should include a physical exam, blood work for key hormones (FSH, LH, AMH, thyroid), and a discussion of your and your partner's medical history.
Step 3: Get Your Partner Involved Immediately
The biggest mistake couples make is having the woman go through months of testing before checking the man. A semen analysis is non-invasive, relatively inexpensive, and provides crucial information fast. It can rule out or identify a major factor right away. Frame it as a team effort: "Let's both get checked so we have the full picture."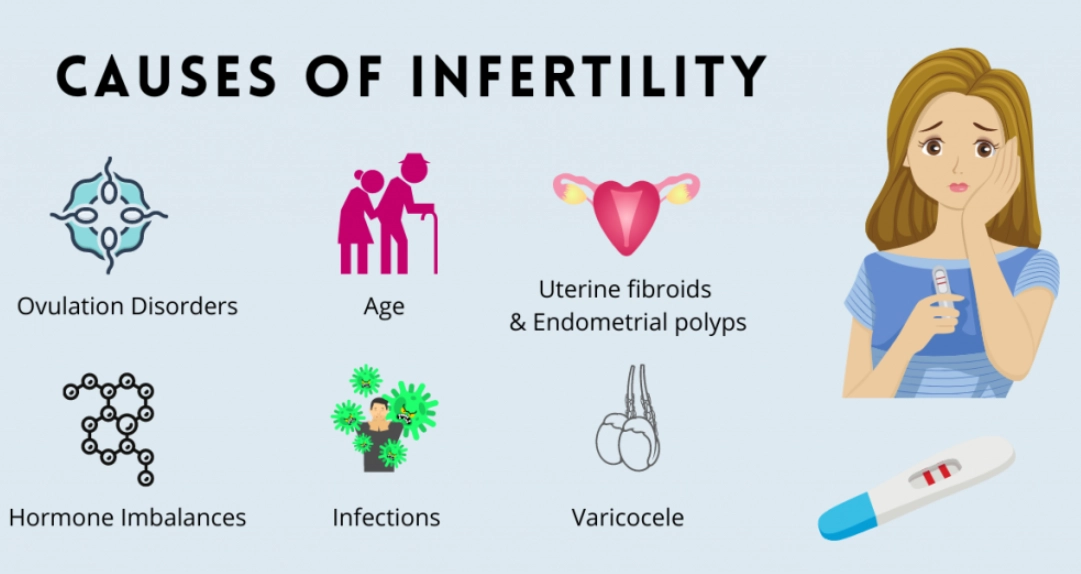
How Do Doctors Diagnose Fertility Issues?
If initial checks point to a problem, you'll move into a more structured fertility evaluation. It's like a puzzle—each test adds a piece.
| Test Type | What It Checks For | What to Expect |
|---|---|---|
| Comprehensive Hormone Panel | Ovulation function, ovarian reserve (egg supply), thyroid health, prolactin levels. | Blood draw, usually on specific days of your cycle (e.g., day 3). |
| Hysterosalpingogram (HSG) | Whether your fallopian tubes are open and if the uterine cavity is a normal shape. | An X-ray procedure where dye is injected through the cervix. Can be briefly uncomfortable. |
| Transvaginal Ultrasound | Uterine fibroids, polyps, ovarian cysts, antral follicle count (a measure of reserve). | A probe is inserted into the vagina. Painless, takes about 15-20 minutes. |
| Semen Analysis | Sperm count, motility (movement), morphology (shape). | Sample produced via masturbation at home or clinic. |
| Laparoscopy (if needed) | Endometriosis, pelvic adhesions, tubal blockages not seen on HSG. | Surgical procedure under anesthesia. Used for both diagnosis and treatment. |
The goal is to build a complete picture. You might find one clear issue, or a combination of minor factors. Sometimes, everything comes back "normal," leading to a diagnosis of "unexplained infertility," which is frustrating but still a valid diagnosis that guides treatment options like IUI or IVF.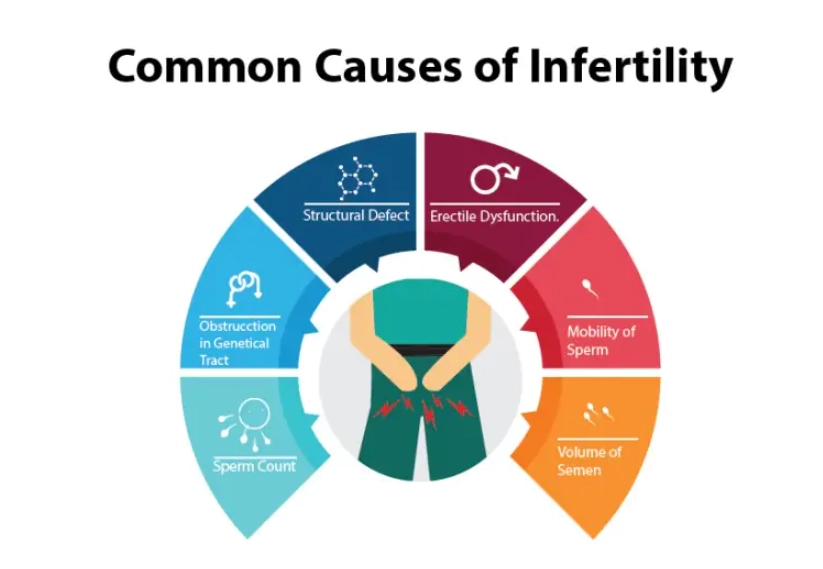
Your Fertility Questions, Answered
My cycles are regular, so I must be ovulating, right?
Regular cycles strongly suggest ovulation, but it's not a guarantee. You can have a regular bleed without releasing a mature egg (anovulatory cycle). The only at-home ways to confirm ovulation are a sustained temperature shift on a BBT chart or a positive urine ovulation predictor kit (OPK) followed by a period about two weeks later. If in doubt, ask your doctor for a progesterone blood test 7 days before your expected period.
We're both young and healthy. Could we still have fertility problems?
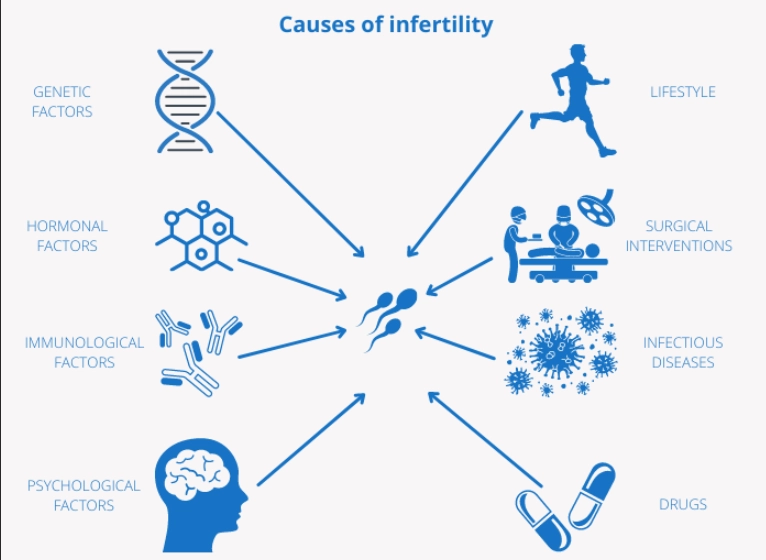
Absolutely. Health and fertility are related but not the same. You can be a marathon runner with impeccable diet and still have a tubal blockage from a past, silent infection. Your partner could be incredibly fit but have a genetic condition affecting sperm production. Age reduces the odds, but specific anatomical or physiological issues can affect anyone.
 How much do basic fertility tests cost, and will insurance cover them?
How much do basic fertility tests cost, and will insurance cover them?
This is the messy part. Coverage varies wildly. A basic hormone panel and semen analysis might cost a few hundred dollars out-of-pocket. An HSG can be $800-$2,000. The first step is to call your insurance company and ask specifically about "diagnostic fertility testing" coverage. Get the CPT codes from your doctor's office. Many plans cover the diagnosis but not the treatments. Don't let cost deter you from initial testing—knowing the problem is the first step to solving it, and you can't make a plan in the dark.
I'm terrified of what we might find. Is it better not to know?
I hear this fear all the time. The uncertainty of not knowing is almost always more stressful than having a clear diagnosis, even if the news is hard. A diagnosis gives you a path—options, next steps, a community of people with the same issue. The "not knowing" space is where anxiety and blame thrive. Knowledge, even difficult knowledge, gives you back control.
Are there things I should stop or start doing right now while we're trying?
Focus on the big three. For both partners: cut back significantly on alcohol and quit smoking (tobacco and recreational drugs). For men, avoid hot tubs and tight underwear if there's a suspected sperm issue—heat is the enemy. For women, aim for a healthy BMI; both underweight and overweight can disrupt ovulation. But don't launch into a crazy crash diet—extreme stress on the body is counterproductive. Think steady, sustainable changes. And take a prenatal vitamin with folic acid now, not after you're pregnant.
 The journey from wondering "How do I know?" to getting answers can feel overwhelming. But each sign you recognize, each test you take, each conversation you have is a move from passive worry to active problem-solving. Your body's signals are worth investigating. Start with one step—maybe tracking your next cycle or making that doctor's appointment. The path to understanding your fertility begins with listening to those whispers and having the courage to seek the answers.
The journey from wondering "How do I know?" to getting answers can feel overwhelming. But each sign you recognize, each test you take, each conversation you have is a move from passive worry to active problem-solving. Your body's signals are worth investigating. Start with one step—maybe tracking your next cycle or making that doctor's appointment. The path to understanding your fertility begins with listening to those whispers and having the courage to seek the answers.




Leave a comment