What You’ll Learn in This Guide
Let’s cut straight to the chase. If you’re searching for endometriosis causes, you’re probably frustrated by vague answers or conflicting information. I’ve spent years talking to gynecologists and patients, and one thing is clear: the causes of endometriosis are more complex than most people realize. It’s not just about “bad periods” or genetics—it’s a mix of factors that interact in ways we’re still figuring out. In this article, I’ll break down the key theories, share some insights you won’t find in typical health blogs, and help you understand what might be behind this condition.
What Exactly is Endometriosis?
Endometriosis is a condition where tissue similar to the lining of the uterus grows outside the uterus, often on the ovaries, fallopian tubes, or pelvic lining. This tissue behaves like regular endometrial tissue—it thickens, breaks down, and bleeds with each menstrual cycle—but since it has no way to exit the body, it causes inflammation, pain, and sometimes scarring. According to the World Health Organization, it affects roughly 10% of women globally, but many cases go undiagnosed for years. The causes are multifaceted, and that’s what makes it tricky to pin down.
The Leading Theories on What Causes Endometriosis
Researchers have proposed several theories to explain endometriosis causes. None of them fully account for every case, which is why it’s often a combination. Here are the big ones.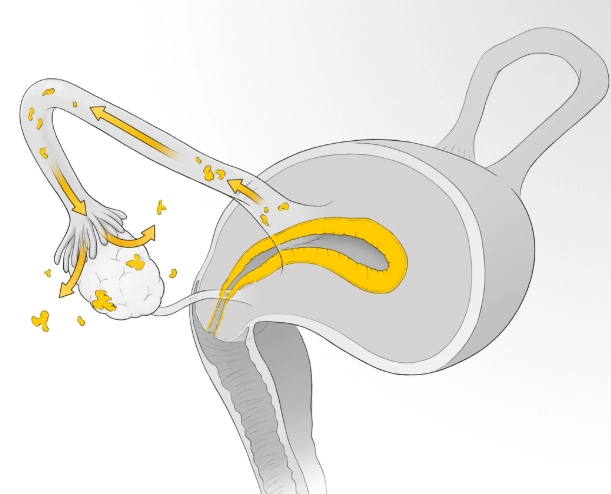
Retrograde Menstruation – The Most Discussed Theory
This is the classic theory you’ve probably heard. During menstruation, some menstrual blood flows backward through the fallopian tubes into the pelvic cavity instead of out of the body. This blood contains endometrial cells that can implant and grow on pelvic organs. But here’s the catch: retrograde menstruation happens in most women, yet only some develop endometriosis. So why? It suggests other factors, like immune system issues, play a role. In my chats with specialists, many point out that this theory alone is too simplistic—it’s like blaming rain for a flood without considering the broken dam.
Genetic Predisposition: Is It in Your DNA?
If your mother or sister has endometriosis, your risk increases significantly. Studies, including those referenced by the Mayo Clinic, show that genetics account for about 50% of the risk. Specific genes related to hormone regulation and inflammation might be involved. But genetics isn’t destiny. I’ve met patients with no family history who still develop severe cases, which hints at environmental triggers.
Immune System’s Role: Why Your Body Might Be Failing
This is where things get interesting. A healthy immune system should clear out misplaced endometrial cells. In endometriosis, the immune system might fail to do that, allowing the cells to thrive. Some research suggests that women with endometriosis have higher levels of inflammatory cytokines—proteins that promote inflammation. It’s not just a reproductive issue; it’s an immune dysfunction. One gynecologist told me that overlooking this is a common mistake—patients often focus on hormones alone, but immune health is crucial.
Environmental and Lifestyle Factors
Exposure to certain chemicals, like dioxins found in some plastics, might increase risk. Diet and stress could also play a part, though the evidence is mixed. For instance, a high-inflammatory diet (think processed foods) might worsen symptoms. I recall a patient who saw improvements after reducing dairy and gluten, but that’s anecdotal—more research is needed.
Risk Factors: Who is More Likely to Develop Endometriosis?
Knowing the risk factors helps identify potential causes. Here’s a table summarizing the key ones based on clinical data.
| Risk Factor | Description | Why It Matters |
|---|---|---|
| Family History | Having a first-degree relative with endometriosis | Increases risk by up to 7 times, per genetic studies |
| Early Menarche | Starting periods before age 11 | Longer exposure to menstrual cycles may contribute |
| Short Menstrual Cycles | Cycles less than 27 days | More frequent periods might raise retrograde menstruation chances |
| Never Giving Birth | Nulliparity or delayed pregnancy | Pregnancy can suppress endometriosis, so lack of it might be a factor |
| High Estrogen Levels | Conditions like obesity or hormone therapy | Estrogen fuels endometrial tissue growth |
Notice how these factors intertwine. For example, genetics might lead to early menarche, which then combines with immune issues. It’s rarely one thing.
Debunking Myths: What Doesn’t Cause Endometriosis
Let’s clear up some confusion. Endometriosis is not caused by sexual activity, poor hygiene, or using tampons. I’ve heard these myths from patients, and they only add to the stigma. Another misconception: it’s just “bad cramps.” That downplays the systemic nature—it can affect the lungs or brain in rare cases. Also, stress doesn’t directly cause endometriosis, but it might exacerbate symptoms by affecting inflammation. A specialist once told me that blaming stress alone is a red flag for misdiagnosis.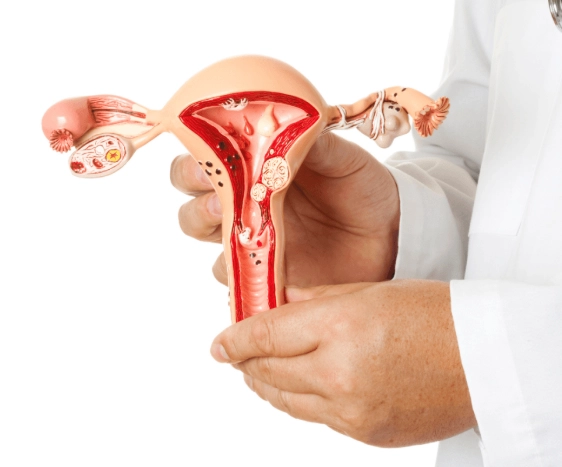
How Endometriosis Develops: A Step-by-Step Explanation
Imagine a typical scenario. Sarah, a 25-year-old, has a genetic predisposition from her mother. She started periods early at age 10. Each month, retrograde menstruation occurs, but her immune system, weakened by chronic stress and a diet high in sugar, fails to clear the stray cells. Over years, these cells implant on her ovaries, causing inflammation and pain. By her late 20s, she’s diagnosed after struggling with infertility. This step-by-step process shows how causes accumulate—it’s a cascade, not a single event.
Here’s a simplified breakdown:
- Step 1: Genetic or environmental trigger sets the stage.
- Step 2: Retrograde menstruation introduces endometrial cells to the pelvis.
- Step 3: Immune dysfunction allows cells to implant and grow.
- Step 4: Inflammation and scarring develop, leading to symptoms.
This isn’t linear—steps can overlap or vary. That’s why treatment often targets multiple areas, like reducing inflammation with diet or medications.
Frequently Asked Questions
Wrapping up, understanding endometriosis causes requires looking at the whole picture—genetics, immune function, environment, and more. It’s not a single culprit but a network of factors. If you’re dealing with this, focus on comprehensive care: talk to a specialist, consider lifestyle tweaks, and don’t buy into quick fixes. The research is evolving, and new insights, like those from the Endometriosis Foundation of America, keep shedding light on this condition. Stay informed, and trust your body’s signals.



Leave a comment